Anchor Composite Resin: a clinical review
I am a general dental practitioner with about twenty years of experience. I am mostly a restorative dentist who has been using composite resin extensively with a direct and indirect approach and as a restorative material after root canal treatment, that is a large part of my activity.
I received a pre-production sample of the Anchor composite resin and I tried it on several clinical cases during a period of about four weeks. What follows is an honest review, and I make it clear in advance that I am not in any way financially related to the group of people involved in the project.
General Overview:
The choice has been to have a sensible number of dentin shades and just two shades of enamel. This is in line with other popular composite resin in the market and gives a relatively easy shade guide to pick our colour from.
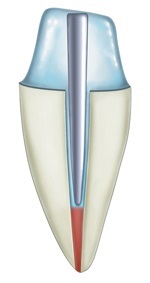
Anterior Composite restorations:
The relatively small number of shades available make it easy to pick your resin. The material is excellent for being easy to handle: it does not stick to the instrument and can be sculpted quickly and effectively. The downsides becomes apparent after final polishing: it can be polished up to a point but with less luster than other brands, due to the well known weakness of hybrid resins compared to microfilled. The bottom line: works well for small/average class 3, less for large class 4.
Posterior Composite restorations:
This is where the Anchor gives its best. After proper isolation restoring posterior teeth, even large cavities, is really simple and straight forward. The use of sectional dental matrix allows to get a tight interproximal contact all the times, and a simple two layers technique (one dentin and one enamel shades) results in excellent aesthetics. The easy handling reduces considerably the operative time: thumbs up!
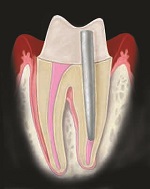
Post Endodontic restorations:
Being root canals a large part of my activity the problem of restoring the tooth with an alternative to a full crown, often for financial issues, is a recurrent dilemma I share with many colleagues. The ability to complete very large composite restoration in a reasonable time suggested to me to try to build onlays with a direct approach: I have to say it was feasible and not in the boundaries of “heroic dentistry”.
It definitely helps to make root canal easy and effective compared with dental implants.
Imaging documentation will follow in a future post
Dr A Frontera, DDS (London)
Il tuo dentista italiano a Londra
afdentist.com